Detecting diabetic eye disease early helps prevent vision loss

Working with Mile Bluff’s chief medical officer Dr. Timothy Bjelland, Liu helped primary care clinics learn to use a retinal camera to take photos of patients’ eyes during routine diabetes checkups. The clinics then send the images to specialists at UW Health, who review and recommend follow-up care for patients who show signs of diabetic retinopathy. This type of screening service, known as teleophthalmology, is critical for patients with less access to eye care specialists.
Beginning in 2015, Liu has conducted research to track the program’s impact over time and identify the barriers and opportunities presented by teleophthalmology. She developed a coaching program called I-SITE to help primary care clinics better integrate this screening technology into their daily work. She also set up a Diabetes Patient Advisory Council in Mauston to engage with patients and gather their input on effective ways to educate and inform the community.
Jeri Shultis joined Liu’s patient advisory council in 2017. He had been proactive in managing his diabetes since his diagnosis, and wanted to help get the word out about the screenings.
Shultis described how the advisory committee arranged for the retinal camera to be on-site to provide free demonstrations at Mauston’s monthly Sharing Supper, a community dining experience intended to build relationships “free of social or economic barriers.”
“Our committee helped explain to community members how the camera worked. It’s not hard at all, and you don’t have to have your eyes dilated,” he recalled.
To date, more than 2,000 patients have received vision-saving eye care as a result of the screening program at Mile Bluff Medical Center. Screening rates, below the national average when the program started, increased substantially to the top quartile nationally.
“Feedback has been very positive,” said Liu. “Primary care clinicians and patients have appreciated it, because it is often difficult to get people in to see an eye doctor. Getting screened the same day you are already in the primary care clinic is helpful to everyone.”
In 2021, with funding from the National Eye Institute, Liu launched a clinical trial at 12 other rural clinics around the country, to determine whether the success at Mile Bluff Medical Center could be replicated elsewhere. In addition to Fort HealthCare and Reedsburg Area Medical Center in Wisconsin, her team works with health systems in Alabama, California, Colorado, New York, Ohio, Tennessee and Vermont. What works for one clinic may not work for others, and Liu’s team wants to understand as much as possible about the barriers, as well as the opportunities for success.
Ultimately, Liu would like to see teleophthalmology become standard at every primary care clinic in the country. She would also like to see Wisconsin leading the nation with the highest screening rates for diabetic eye disease and the lowest rates of diabetes-related blindness. The goal builds on a UW legacy: The international guidelines for treating diabetic eye disease were developed at UW–Madison, thanks to a 1970s study led by Dr. Matthew “Dinny” Davis.
“We have known for 50 years that we can treat this disease, and it’s still the leading cause of blindness in this country,” Liu said. “That’s mostly due to lack of screening.”

Addressing that lack means testing new ways of making screening more efficient and effective. Approximately twenty to thirty percent of diabetes patients screened for eye disease require referral to a specialist who may perform interventions such as injections in the eye, laser treatments or surgery. For these patients, time is of the essence. Dr. Roomasa Channa, an associate professor of ophthalmology, studies a screening method that relies on artificial intelligence (AI) to provide immediate results. Unlike standard teleophthalmology, where a primary care clinic sends images to eye specialists elsewhere, an AI-based teleophthalmology program reads the image as soon as it’s taken.
“Because the tool can recognize the distinctive hallmarks of diabetic retinopathy, the clinician can tell the patient right away whether or not they have referrable disease,” Channa said.
This increases the likelihood, she said, that patients will follow up with recommended eye care. In medically underserved areas, once patients leave the office, clinicians can lose contact with them for extended periods. Channa’s lab developed a strategy called AI-BRIDGE that incorporates culturally adapted patient education and helps local clinics schedule appropriate follow-up eye appointments for patients. In August 2024, she was approved for a national clinical trial funded by the National Institutes of Health (NIH) and the National Eye Institute to test the effectiveness of AI-BRIDGE at nine clinics around the country.
Last month, the NIH purported to terminate the funding opportunity for the award. Wisconsin is a plaintiff in a multi-state lawsuit aimed at reinstating terminated NIH grants, and the fate of the funding for Channa’s grant is uncertain at the time of this story’s publication.
“Wherever diabetes is increasing, so is diabetic retinopathy,” said Channa. “This broadly impacts people living in medically underserved communities. As one example, here in Wisconsin, our Native and Hispanic populations are more likely to have limited access to health care and have growing rates of diabetes. This leaves them particularly vulnerable to severe complications like blindness.”
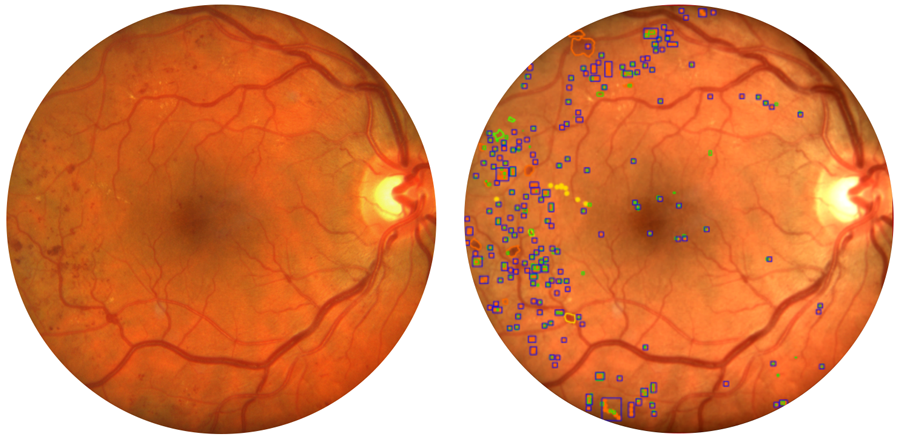
Channa said that both standard teleophthalmology and AI-based programs offer busy clinicians options based on what works best for them, their clinics and their patients.
Liu and Channa collaborate on research to promote improved vision outcomes and share the goal of helping patients recognize the importance of screenings and treatment.
“People living in medically underserved communities need a voice,” said Channa. “Everyone deserves access to the best medical expertise our country has to offer. This research is aimed at providing efficient, effective diabetic retinopathy screening to communities that currently have the worst outcomes. Our goal is to use innovative systems to save sight.”
Research at the University of Wisconsin–Madison drives innovation, saves lives, creates jobs, supports small businesses, and fuels the industries that keep America competitive and secure. It makes the U.S. — and Wisconsin — stronger. Federal funding for research is a high-return investment that’s worth fighting for. Learn more about the impact of UW–Madison’s federally funded research and how you can help.
link